Fax: 770-339-9804
Lawrenceville, Georgia 30046

Finishing treatment for breast cancer is powerful.
It’s the surgery.
The appointments.
The treatments.
The resilience you had to find inside yourself.
And then comes the quiet question many women carry:
“What is my risk of breast cancer recurrence?”
If that thought crosses your mind — even years later — you’re not alone.
Breast cancer recurrence is one of the most common and emotionally challenging concerns for survivors. Even after successful treatment, the possibility of cancer returning can create lingering anxiety. Understanding what recurrence means, the different types and subtypes, common symptoms, and recommended follow-up care can empower survivors to take an active role in their health.
Dr. Schwartz believes confidence comes from clarity. When you understand your recurrence risk, follow a structured breast cancer survivorship plan, and have a surgeon who continues walking with you long after surgery, fear loses its power.
Breast cancer recurrence occurs when cancer returns after treatment and a period during which it was undetectable. Recurrence happens because small clusters of cancer cells may survive initial treatment. These cells can remain dormant for months or even years before becoming active again.
Recurrence is different from a new primary breast cancer. A recurrence originates from the original cancer, while a new primary cancer develops independently.
Breast cancer can recur:
The risk of recurrence depends on multiple factors, including tumor size, lymph node involvement, hormone receptor status, HER2 status, tumor grade, and response to treatment.
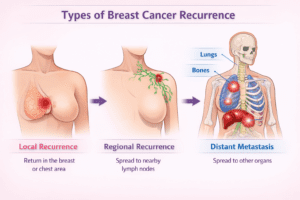
Understanding the different types of recurrence helps clarify prognosis and treatment options.
Local recurrence occurs in the same breast (after lumpectomy) or in the chest wall (after mastectomy).
Local recurrence is often treatable, especially when detected early. Because Dr. Schwartz performs both the oncologic surgery and the reconstruction, he has a detailed understanding of your surgical anatomy — which allows for careful, precise long-term monitoring of the operative area.
Regional recurrence affects nearby lymph nodes.
Lymph node involvement at the time of diagnosis can increase recurrence risk, which is why sentinel lymph node biopsy and axillary evaluation are essential components of comprehensive breast cancer surgery. Treatment typically involves a combination of surgery, radiation, systemic therapy, or targeted treatments.
Distant recurrence means the cancer has spread to organs beyond the breast and nearby lymph nodes. This stage is also called metastatic breast cancer or Stage IV.
Bone metastasis:
Liver metastasis:
Lung metastasis:
Brain metastasis:
While metastatic breast cancer is more complex, treatment advances continue to improve survival and quality of life. Early recognition remains critical. Although metastatic breast cancer is not considered curable, it is treatable, and many patients live for years with ongoing therapy.
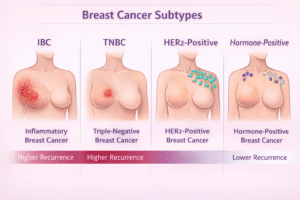 Breast cancer is not a single disease, and not all breast cancers behave the same. Subtypes significantly influence recurrence patterns and timelines.
Breast cancer is not a single disease, and not all breast cancers behave the same. Subtypes significantly influence recurrence patterns and timelines.
These cancers grow in response to estrogen or progesterone.
Hormone receptor-positive cancers tend to have a lower early recurrence rate but a longer risk window.
HER2-positive cancers overexpress the HER2 protein, which promotes rapid growth.
Thanks to targeted HER2 therapies, recurrence rates have dropped dramatically. Still, structured breast cancer follow-up care remains essential.
Triple-negative breast cancer lacks estrogen receptors, progesterone receptors, and HER2.
TNBC tends to be more aggressive, but if no recurrence occurs within five years, the long-term outlook improves significantly.
This rare and aggressive form often presents without a distinct lump.
Individuals with inherited mutations may face higher recurrence and new cancer risks. Genetic counseling can guide surveillance and prevention strategies.
Recurrence can occur:
Most recurrences happen within the first five years, but long-term vigilance remains important.
Certain factors increase the likelihood of recurrence:
While some factors are beyond control, lifestyle modifications, such as maintaining a healthy weight, staying physically active, limiting alcohol, and avoiding tobacco, can help reduce the risk of recurrence.
But here is something important :
Recurrence is not caused by one stressful week.
It is not caused by one missed workout.
It is not your fault.
Breast cancer biology — not guilt — drives recurrence.
One of the unique aspects of Dr. Schwartz’s approach is his “one surgeon, one surgery” model.
Rather than separating cancer removal and reconstruction into different surgical teams, Dr. Schwartz performs both the oncologic breast surgery and the reconstructive procedure in a single coordinated operation whenever appropriate.
Why does this matter for breast cancer recurrence and survivorship?
This continuity provides both medical precision and emotional reassurance.
You’re not starting over with a new doctor after cancer treatment ends. You continue with the same surgeon who guided you from diagnosis through reconstruction and into survivorship.
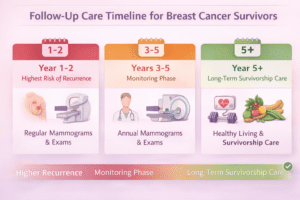
Follow-up care is essential not only for detecting recurrence early and managing long-term side effects but for your peace of mind as well.
Most survivors follow this schedule:
Your doctor will:
Annual mammograms are recommended for:
After mastectomy, imaging may not be necessary unless symptoms arise.
Routine full-body scans are not typically recommended unless symptoms suggest recurrence. Unnecessary imaging can cause anxiety and false positives.
Routine tumor marker tests are not universally recommended but may be used in certain cases.
Some patients take:
Dr. Schwartz personalizes surveillance recommendations based on tumor biology, surgical history, genetics, and overall risk profile.
This is not a “one-size-fits-all” plan. It is tailored breast cancer survivorship care.
Recognizing early warning signs is critical. Symptoms vary depending on recurrence type.
Being informed is empowering – not frightening.
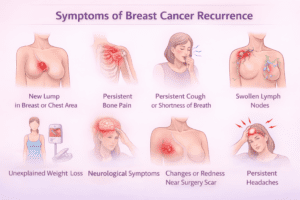
If you notice persistent new symptoms, scheduling an evaluation is the right step. Most concerns turn out to be benign — but reassurance is valuable.
While recurrence cannot be completely prevented, evidence-based strategies help lower risk.
Exercise has been shown to reduce recurrence risk and improve overall survival.
Fear of recurrence is common among survivors. This anxiety can surface before follow-up appointments, anniversaries of diagnosis, or when experiencing new symptoms.
Healthy coping strategies include:
Mental health is as important as physical health in survivorship.
Breast cancer survivorship is about more than scans and lab tests.
It’s about:
At mybreastcancerdoc.com, survivorship is an extension of your original care — not a separate phase where you’re left to navigate alone.
Because Dr. Schwartz combines advanced breast oncology and reconstructive surgery expertise, patients benefit from coordinated care that protects both their health and their sense of wholeness.
You are not just a cancer case.
You are a woman with a future — and that future deserves thoughtful, proactive guidance.
Recurrence risk depends on your cancer type, stage, and treatment.
For many women, the risk of breast cancer recurrence is highest within the first two to five years after diagnosis.
However, hormone receptor–positive breast cancer can recur many years later. That’s why long-term follow-up care and, in some cases, extended hormone therapy are recommended.
Your oncologist can provide personalized estimates using pathology reports and predictive tools.
There is no strong evidence that stress directly causes recurrence. However, chronic stress can affect overall health, so stress management is beneficial.
Yes, breast cancer can recur after a mastectomy, although the risk is generally low.
Recurrence after mastectomy most commonly occurs in the chest wall or nearby lymph nodes. This is why routine follow-up exams remain important even after full breast removal and reconstruction.
No. Breast reconstruction does not increase the risk of breast cancer recurrence.
When reconstruction is performed by an experienced surgeon who prioritizes oncologic safety — such as in Dr. Schwartz’s comprehensive “one surgeon, one surgery” approach — cancer removal and reconstruction are carefully coordinated to protect both health and aesthetic outcomes.
Symptoms depend on where it spreads. Persistent pain, neurological changes, chronic cough, or unexplained weight loss should be evaluated promptly.
Not necessarily. Cancer biology is complex. Some microscopic cells may survive despite appropriate treatment.
Many people live long, fulfilling lives with metastatic breast cancer.
Routine scans are not recommended unless symptoms arise. Over-scanning can lead to unnecessary anxiety and false alarms.
No specific diet guarantees prevention. However, plant-based diets, reduced alcohol intake, and weight management are associated with improved outcomes.
Yes. Hormone therapy significantly reduces recurrence risk in hormone receptor-positive breast cancer.
Five years without recurrence is an important milestone, especially for triple-negative breast cancer. However, hormone receptor-positive cancers may recur later, so long-term follow-up remains important.
Many women can safely become pregnant after treatment. Timing and safety depend on cancer subtype and treatment history. Consult your oncologist.
A survivorship plan should include:
Strategies include:
Medical research continues to improve outcomes.
Recent advances include:
These innovations help tailor treatments and reduce unnecessary therapy.
Breast cancer recurrence is possible. But it is not inevitable.
With comprehensive surgical care, integrated reconstruction, and structured survivorship planning, you can move forward informed — not afraid. Recurrence fear may never disappear entirely—but knowledge, vigilance, and support can transform fear into empowerment.
Breast cancer recurrence is a complex and deeply personal experience. While the possibility of recurrence can feel overwhelming, understanding the types, subtypes, symptoms, and follow-up care empowers survivors to stay proactive.
Modern medicine has significantly improved outcomes, and early detection of recurrence can expand treatment options. Maintaining regular follow-up appointments, adhering to prescribed therapies, adopting healthy lifestyle habits, and seeking emotional support all contribute to long-term well-being.
The healthiest approach is balanced:
Survivorship is a journey—not just of vigilance, but of resilience. By staying informed and connected to your care team, you can move forward with confidence and clarity.
If you are a survivor concerned about recurrence, speak openly with your healthcare provider. Personalized guidance is the most powerful tool in navigating life after breast cancer.
 Dr. Schwartz is a highly respected national leader in oncoplastic breast surgery. He is a preferred provider for the majority of insurance plans and is highly recommended by insurance companies and patients alike. By performing most of his surgeries in an outpatient ambulatory center, he saves his patients on hospital costs, co-pays, and more.
Dr. Schwartz is a highly respected national leader in oncoplastic breast surgery. He is a preferred provider for the majority of insurance plans and is highly recommended by insurance companies and patients alike. By performing most of his surgeries in an outpatient ambulatory center, he saves his patients on hospital costs, co-pays, and more.
As a breast surgeon and reconstructive surgeon, he performs most mastectomies and reconstructions in one surgery, saving his patients time and money by seeing only one expert, paying only one set of deductibles and co-pays, and most importantly, reducing time spent in the operating room while providing unparalleled results.
Dr. Schwartz and his entire staff specialize in breast surgeries only, and as such, are highly experienced in dealing with insurance companies. They can provide guidance and invaluable information to women undergoing breast reconstructive surgeries. Additionally, as part of the Northside Hospital system, patients benefit beyond Dr. Schwartz’s practice.
Dr. Schwartz is always accepting new patients diagnosed with breast cancer and makes it his priority to see them immediately, despite his very busy schedule.
Click to SCHEDULE YOUR CONSULTATION TODAY!